If you or someone you love is living with diabetes, you’re probably already managing a lot, with blood sugar levels, diet, medication and regular medical checkups. Dental health may not be at the top of that list. But here’s something that surprises many of our patients at Nairobi Sterling Dental Clinic: the mouth and diabetes are far more closely connected than most people realise.
It’s not a one-way relationship either. Diabetes affects the health of your mouth, and poor oral health can, in turn, make diabetes harder to manage. Understanding this connection could genuinely change how you approach both conditions and your overall quality of life. Let’s explore what the research tells us, what to watch out for, and what you can do about it.
How Diabetes Affects Your Oral Health
When blood sugar levels are poorly controlled, the effects are felt throughout the body. The mouth is no exception. Here’s how diabetes can directly impact your oral health:
Increased risk of gum disease.
This is the most significant and well-documented connection. People living with diabetes have a reduced ability to fight bacterial infections, including those in the gums. This makes them significantly more susceptible to gingivitis, the early stage of gum disease, and to its more serious form, periodontitis. Gum disease also tends to be more severe and progress more quickly in people with diabetes than in those without.
Slower healing.
If you’ve had a tooth extraction, a dental procedure, or even a small mouth injury, diabetes can slow down the healing process. Reduced blood flow and a compromised immune response mean that wounds in the mouth take longer to heal and are more vulnerable to infection.
Dry mouth.
Diabetes can reduce saliva production, leading to a persistently dry mouth. As we’ve discussed in our article on bad breath, saliva is essential for washing away food particles, neutralising acids, and keeping bacteria in check. Without enough of it, the risk of tooth decay, gum disease, and bad breath all increases.
Thrush and fungal infections.
High glucose levels in saliva create an environment where fungi, particularly Candida, can thrive. Oral thrush, which presents as white or red patches in the mouth, is more common in people with diabetes, especially those whose blood sugar is not well controlled.
Burning mouth sensation.
Some people with diabetes experience a burning or tingling sensation in the mouth, lips, or tongue. This can be related to nerve damage, which is a complication of long-term uncontrolled diabetes. It could also be attributed to dry mouth and fungal infections.
Greater risk of cavities.
Elevated glucose in saliva feeds the bacteria responsible for tooth decay. Combined with dry mouth and reduced immunity, this creates conditions where cavities develop more readily and more quickly.
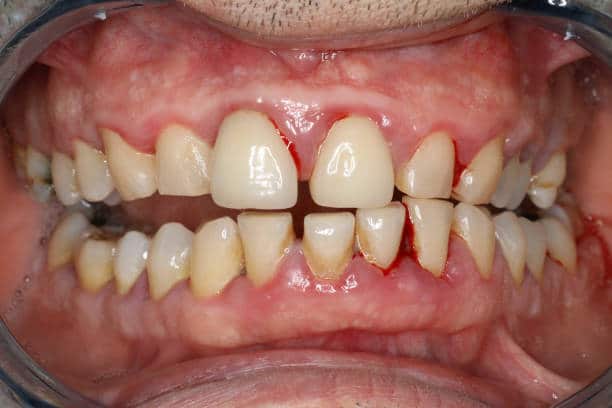
The Other Direction: How Gum Disease Affects Diabetes
This is the part that often surprises people the most. The relationship between gum disease and diabetes doesn’t just run one way. Gum disease can actively make diabetes harder to control.
Here’s why: gum disease is an infection, and like any infection in the body, it triggers an inflammatory response. This inflammation interferes with the body’s ability to use insulin effectively, which can cause blood sugar levels to rise. For someone already managing diabetes, persistent gum disease can make blood sugar control significantly more difficult. This creates a frustrating cycle where each condition worsens the other.
Research has shown that treating gum disease in people with diabetes can lead to measurable improvements in blood sugar control. In other words, taking care of your gums isn’t just good for your mouth. It could make a real difference to your diabetes management.
This is a powerful reason why dental care should be considered an essential part of diabetes management, not an optional extra.
Signs to Watch Out For
If you have diabetes, be particularly vigilant about the following oral health warning signs:
- Gums that bleed when you brush or floss
- Red, swollen, or tender gums
- Gums that appear to be pulling away from the teeth
- Persistent bad breath that doesn’t improve with brushing
- A dry, sticky feeling in the mouth
- White or red patches inside the mouth
- Teeth that feel loose or have shifted
- Slow-healing sores or wounds in the mouth
- A burning or tingling sensation on the tongue or lips
Any of these symptoms warrants a dental visit, ideally sooner rather than later.
Practical Steps for People with Diabetes
Managing your oral health when you have diabetes doesn’t require a completely different approach. It requires a more consistent and attentive one. Here’s what makes the biggest difference:
Keep your blood sugar as well-controlled as possible.
This is the single most impactful thing you can do for your oral health. Better blood sugar control reduces your susceptibility to gum disease, speeds up healing, and lowers your risk of oral infections. Your mouth and your body will thank you.
Brush thoroughly, twice a day.
Use a soft-bristled toothbrush and fluoride toothpaste. Be gentle but thorough. Pay close attention to the gumline where bacteria tend to accumulate most.
Floss every day.
Removing plaque and food debris from between the teeth is especially important when you have diabetes. The spaces between teeth are prime territory for the bacteria that cause gum disease.
Stay well hydrated.
Drinking plenty of water helps combat dry mouth, keeps saliva flowing, and supports the mouth’s natural defences against bacteria.
Avoid smoking.
Smoking significantly increases the risk of gum disease in anyone, but in people with diabetes, the combination is particularly damaging. If you smoke and have diabetes, quitting is one of the most beneficial steps you can take for both your oral and general health.
Tell your dentist you have diabetes.
This is important and often overlooked. Your dentist needs to know about your diabetes diagnosis, your current blood sugar control, and any medications you’re taking. This information affects how we plan your treatment, how we manage healing after procedures, and how frequently we recommend you come in. We’re your partners in this. The more we know, the better we can help.
Come in more frequently for checkups.
While most people benefit from a dental checkup every six months, those with diabetes, particularly where blood sugar control is a challenge, may benefit from more frequent visits. Every three to four months is often recommended. More regular professional cleanings help keep gum disease at bay and allow us to catch any developing problems before they escalate.

A Note for Families and Caregivers
If you’re caring for a family member with diabetes, oral health is one area where your support can make a real difference. Helping them maintain a consistent brushing and flossing routine, reminding them to stay hydrated, and ensuring dental checkups don’t get overlooked amid the many other demands of managing diabetes. These are meaningful contributions to their overall health and well-being.
When Should You See a Dentist?
If you have diabetes, you should book a dental appointment if:
- You haven’t had a checkup or professional cleaning in the last three to six months
- You notice any of the warning signs listed above
- Your blood sugar control has been particularly difficult recently
- You’re about to start a new diabetes medication – some can affect oral health
- You have dry mouth, mouth soreness, or any unusual changes in your mouth
- You’re due for a dental procedure and want to discuss how your diabetes may affect healing
Don’t wait for something to hurt. In people with diabetes, the progression from early gum disease to more serious periodontitis can happen faster than average. This makes prompt attention all the more important.
How We Can Help at Sterling Dental
At Nairobi Sterling Dental Clinic, we understand that patients with diabetes need a dental team that is attentive, thorough, and genuinely informed about how their condition interacts with their oral health. We take a personalised approach, assessing not just the current state of your teeth and gums, but the factors that put you at greater risk and the steps we can take together to keep things on track.
For patients with diabetes, we typically recommend more frequent professional cleanings and careful monitoring of gum health. Moreover, we advocate for open communication about your medical management so we can coordinate your dental care accordingly.
Whether you’ve been recently diagnosed or have been managing diabetes for years, it’s never too late to take stock of your oral health and make it part of your broader health routine. Make Sterling Dental Clinic your trusted partner in this journey. Book your consultation with our team at the Park Suites Building in Parklands today. You can also reach out to us on call via +254762 223 925 for enquiries.

